The Gut as Ground Zero
Why gut health is foundational to detoxification, neurological rewiring and long-term recovery from addiction and mental illness
Key Takeaways
- Most of your body's serotonin — the "feel good" chemical — is made in your gut, not your brain.
- Alcohol, opioids, and stimulants all damage the gut's bacterial ecosystem, making cravings and emotional instability worse — even after you've stopped using.
- Healing the gut through food, fibre, probiotics, and sleep is now recognised as essential to lasting recovery.
Addiction is not simply a crisis of willpower or brain chemistry. Emerging science reveals it is, in significant part, a disorder of the gut — and recovery depends on treating it as such.
For decades, addiction treatment focused almost entirely on the brain. But science is proving: your gut plays a massive role in mental health and recovery.
Inside your digestive system lives a vast community of bacteria — your gut microbiome. This community doesn't just help you digest food. It helps regulate your mood, your stress response, your cravings, and even how your brain forms new habits. When it's disrupted, everything from your sleep to your motivation to stay sober can suffer.
A 2024 study published in Neurobiology of Stress found that shifts in gut bacteria can alter neurons in the brain's reward centre — directly affecting how people respond to substances and manage their emotions.
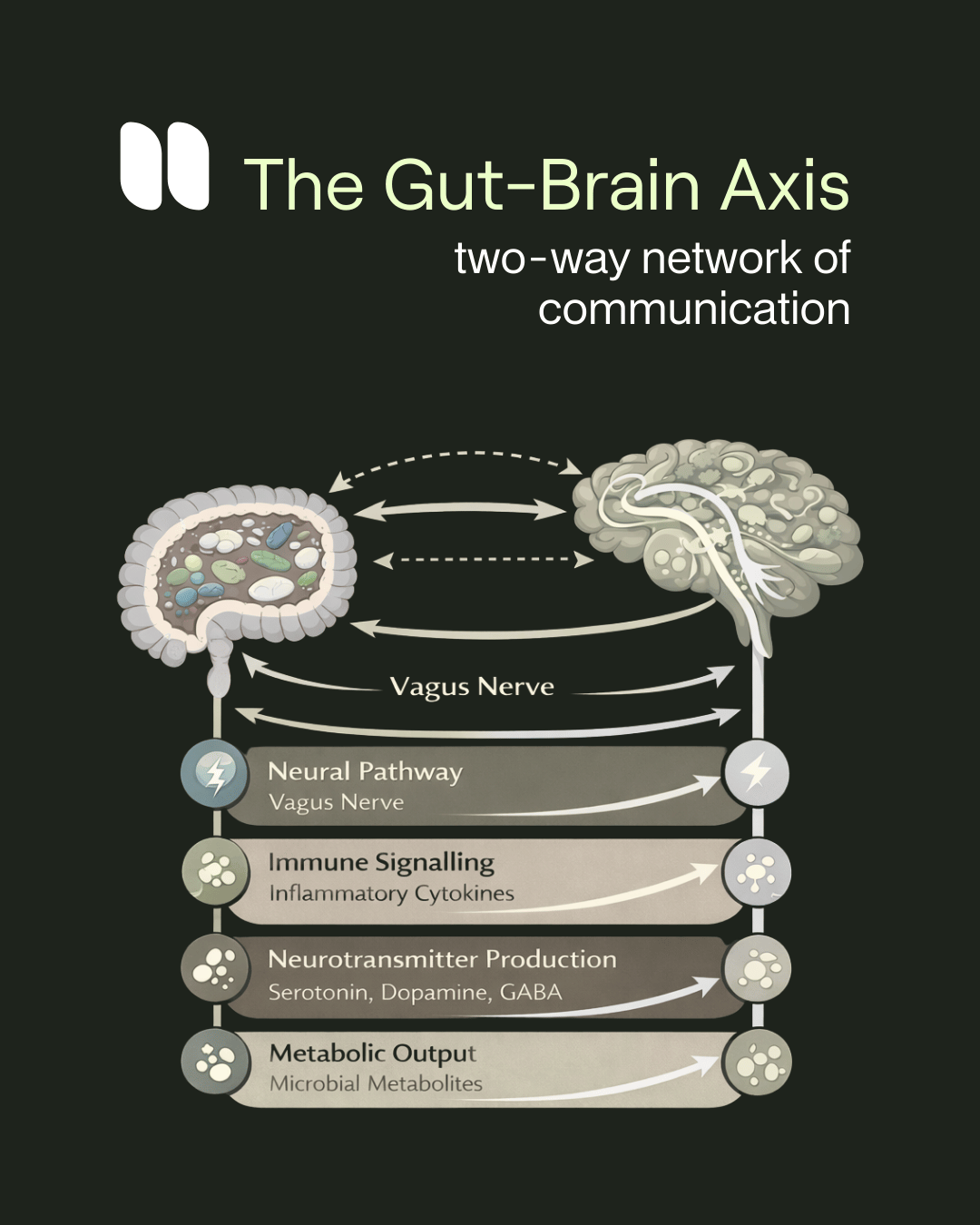
Your Gut and Brain Are in Constant Conversation
Think of the gut and brain as being in constant, two-way communication — like a phone call that never ends. This happens through something called the gut-brain axis, a network of nerves, hormones, and chemical signals.
Here's what makes this so important for recovery:
- Around 90–95% of your body's serotonin — the chemical that regulates mood, sleep, and emotional stability — is produced in the gut, not the brain. When your gut bacteria are out of balance, serotonin production drops.
- Gut microbes also influence dopamine (the brain's reward chemical) and GABA (which calms the nervous system).
- When the gut lining becomes "leaky," harmful substances can escape into the bloodstream and trigger inflammation that reaches the brain — worsening depression, anxiety, and pain sensitivity.
How Substances Damage the Gut
Every major class of substance disrupts the gut microbiome — often significantly, and sometimes before a formal addiction even develops.
- Alcohol:
Makes the gut lining more permeable and reduces the diversity of healthy bacteria. Even binge drinking — before addiction develops — already shows measurable changes in gut bacteria and impaired cognition. - Opioids
Bind to receptors throughout the gut, disrupting its function. Research shows that depleting gut bacteria significantly amplifies cravings for opioids — and restoring them reduces that drive. - Stimulants
Alter gut movement and flood the system with stress hormones that reshape the microbial environment. Depleted gut bacteria have been shown to enhance cocaine-seeking behaviour and increase relapse during withdrawal.
Withdrawal Is a Gut Event Too
Most people think of withdrawal as something that happens in the brain. But it's also happening in the gut — and the two are deeply connected.
During detox, gut permeability worsens and inflammation rises. Those inflammatory signals travel to the brain, driving the anxiety, insomnia, brain fog, and heightened pain that make withdrawal so difficult. Standard detox medications don't address this gut-driven component.
The gut also regulates cortisol — your stress hormone. When the gut is damaged, baseline stress levels stay elevated, making it much harder to manage the triggers that lead to relapse. A 2020 review in Frontiers in Psychiatry found that probiotic and dietary interventions reduced anxiety and depression symptoms with effects comparable to some medications.
"Supporting gut health during and after detox is not complementary care. It is a clinical necessity."
The Gut's Role in Rewiring the Brain
Long-term recovery isn't just about stopping use — it's about the brain building new patterns, new responses, new ways of finding reward. And here's where the gut becomes even more critical.
Microbial metabolites — tiny molecules produced by gut bacteria — can cross the blood-brain barrier and directly influence dopamine signalling. They also regulate the enzymes that produce serotonin. In other words, what's happening in your gut is actively shaping the neurochemical environment in which new habits either take hold or collapse.
Stanford University research published in Cell (2021) found that a diet high in fermented foods increased microbiome diversity and reduced the exact inflammatory markers linked to depression, anxiety, and blunted reward response — in just ten weeks. The protein responsible for brain plasticity (BDNF) is similarly supported by a healthy microbiome. Without healing the gut, the biological foundations for lasting change remain compromised.
What This Means for Treatment
The gut isn't a passive bystander in recovery. It produces the neurotransmitters that regulate your mood. It governs the inflammation that shapes pain and cognition. It determines the neurochemical conditions in which lasting change either takes hold or fails.
Treating addiction without treating the gut is an incomplete intervention. The microbiome doesn't heal itself when you stop using — in many cases, the disruption deepens during withdrawal, exactly when the brain is being asked to start rebuilding.
Further Reading
- The Psychobiotic Revolution — Scott C. Anderson, John F. Cryan & Ted Dinan (book)
- The Mind-Gut Connection — Emeran Mayer, MD (book)
- Huberman Lab — Gut-Brain Axis episodes (podcast)
Scholarly References
García-Cabrerizo, R. & Cryan, J.F. (2024). Neurobiology of Stress, 30, 100629.
Hofford, R.S. & Kiraly, D.D. (2024). Biological Psychiatry, 95(4), 329–338.
Carbia, C. et al. (2023). eBioMedicine (The Lancet), 89.
Pak, R. et al. (2025). Frontiers in Neuroscience.
Wastyk, H.C. et al. (2021). Cell, 184(16), 4137–4153.
Frontiers in Immunology (2024). The microbiota-gut-brain-immune interface in the pathogenesis of neuroinflammatory diseases.
---------------------
INTEGRATED TREATMENT AT NOOSA CONFIDENTIAL
At Noosa Confidential, gut health is embedded within our evidence-based treatment protocols. Our clinical team works across nutrition, neuroscience, and personalised medicine to address the biological foundations of recovery — because lasting change requires more than willpower. It requires a body that is capable of it.
To find out more about our integrated approach, contact our clinical team.